Some People Who Seem to Be in a Coma and Can’t Speak or Move May Actually Be Conscious and Hear Us, New Study Reveals
15 to 20 percent of patients who appear to be in a coma could be aware of their surroundings.
Some people who seem to be in a coma and are speechless and motionless may actually be conscious and aware of their surroundings. It’s called “covert consciousness,” and this week Scientific American examined the phenomenon, what experts know (and don’t know) about it, and how medical care might have to change to deal with it.
The report looked at the case of Maria Mazurkevich, a 30-year-old New Yorker who went into a coma after a blood vessel ruptured in her brain. She was placed on a ventilator, was unresponsive, and seemed to be unaware of her surroundings. But an EEG—sensors that assessed her brain’s electrical activity—told a different story.
While the EEG was placed on her head, doctors told the unconscious woman to “keep opening and closing your right hand” and “stop opening and closing your right hand.” Her hands didn’t move, but her brain’s activity showed she was aware of the instructions and that they were different. Read on to find out more.

Experts believe Mazurkevich was experiencing “covert consciousness,” in which the brain reacts to the outside world with some comprehension, but the body remains unresponsive. As many as 15 to 20 percent of patients who appear to be in a coma exhibit this kind of internal awareness when monitored with technology that can measure brain activity.
This is changing scientists’ understanding of comas and other unresponsive states, Scientific American says. Studies have found that people whose covert consciousness is detected early have a greater chance of full, functional recovery. So experts say it’s important to study and further understand the phenomenon.

“The standard definition of a comatose patient is someone who is unconscious, is unable to be awakened, and has no signs of awareness or the ability to interact with the environment,” says Scientific American. “Patients in a coma caused by severe brain injury may look indistinguishable from someone in a deep sleep, except that most comatose patients cannot breathe on their own and need support from a ventilator, with a tube inserted into their airway.”
But the discovery of covert consciousness has challenged that definition. “The problem with severe brain injury,” said neuroscientist Nicholas Schiff in The Scientist, “is that you have people who all look the same who could have very different trajectories of recovery over time, response to treatment, or already achieved level of recovery.”
In 2006, a neuroscientist gave a brain MRI to a young woman who had experienced a severe traumatic brain injury and was believed to be in a vegetative state. During the scan, doctors asked her to imagine playing tennis and walking through the rooms of her house. The woman’s brain was activated similarly to those of healthy people.
In 2019, the first large study to use EEGs to diagnose covert consciousness was published in the New England Journal of Medicine. Doctors asked patients to move their hands, then analyzed EEG readings to identify brain activity in response. A year later, 44 percent of patients who had some brain activity were no longer vegetative and could function independently.

And in 2017, covert consciousness was detected in seemingly unconscious people who had just been admitted to the ICU with severe brain injuries, suggesting the phenomenon can happen in people who have very recently been hurt.
So developing a diagnostic test to identify covert consciousness is imperative. Scientists are trying to do just that. But it’s been slow going, for a simple reason: No one knows what causes covert consciousness, so no one knows what changes in which area of the brain to look for.
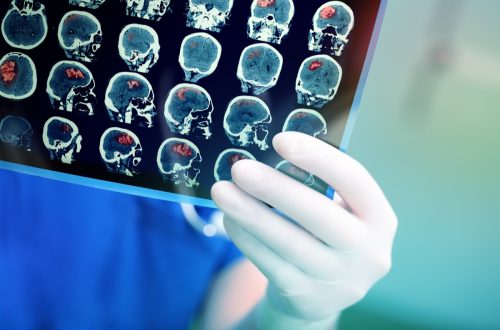
Some studies suggest covert consciousness may be caused by brain injuries that disconnect the thalamus—the part of the brain that conveys movement signals and sensory information—from the cerebral cortex, which is responsible for higher-level cognitive functioning. But injuries in multiple parts of the brain might also cause the condition.
Another complication in testing for covert consciousness: People with severe brain injuries often have fluctuating levels of consciousness. A single test might miss important signs, so experts aren’t sure how often they may need to be tested, says Scientific American.
But it’s becoming clear that covert consciousness is common enough that more answers must be found. “This is very big for the field,” Schiff told The New York Times in 2019 about the New England Journal study. “The understanding that, as the brain recovers, one in seven people could be conscious and aware, very much aware, of what’s being said about them, and that this applies every day, in every I.C.U. — it’s gigantic.”














